Medicare Supplement Basics
A Medicare Supplement is a type of health insurance sold by private insurance companies to cover the gaps in Medicare. Medicare Supplement plans pay after Medicare approves and pays its share of your claim. This includes deductibles, coinsurance and copays. This is typically the remainder of your bill. However, this does depend on which policy you choose out of the standard plans offered. There are 10 standard plans offered. See Compare Medicare Supplement Plans side by side.
Some of the main advantages of a traditional Medicare Supplement policy are:
- Freedom to choose your own doctors and hospitals
- No specialist referrals required
- Predictable out-of-pocket expenses for Medicare-covered services
- Nationwide coverage
- Guaranteed renewable – the insurance company can’t drop you or change your coverage due to a health condition
Medicare Supplemental insurance is the most predictable coverage that you can buy. You will know exactly what’s covered for every inpatient or outpatient procedure based on which Medigap plan you choose.
Keep in mind with Medicare Supplement insurance:
- You must have Medicare Part A and Part B to buy a Medigap policy.
- Medicare supplement plans cover only one person. Your spouse must have his or her own individual policy.
- You can drop your supplement at any time. There is no annual election period for Medicare Supplement plans.
- The annual election period in the fall is for drug plans.
- Many carriers offer household discounts if two or more people enroll in Medicare supplemental plans from the same company.
- Plans do not include Part D, so you’ll add a separate standalone Part D drug plan.
- If you currently have a Medicare Advantage plan, you can switch to a Medicare Supplement policy but make sure you can leave the Medicare Advantage plan before your Medicare Supplement policy begins.

Compare Medicare Supplement Plans Side by Side
Medicare Supplement plans are lettered A – N and each plan covers a different Medicare gap. You can compare Medicare Supplement plans side-by-side using the Medicare Supplement Plans comparison chart below. This makes comparing Medicare Supplement plans pretty simple. Keep in mind Medicare Supplements and Medigap plans are the same thing.
Some Medigap plans will have higher premiums and offer more coverage. Other Medigap plans will have lower premiums since you will pay some of the gaps in Medicare yourself. If you compare Medicare Supplements, you’ll be able to see which plans cover what’s most important to you.
When you compare Medicare Supplement plans in 2022, you’ll find that many name brand carriers you are familiar with are offering these plans.
Keep in mind each insurance company decides which Medigap policy it wants to sell, although state laws might affect which ones they offer. They don’t have to offer every Medigap plan. But, they must offer Medigap Plan A if they offer any Medigap policy and they must offer Plan C or Plan F if they offer any plan.
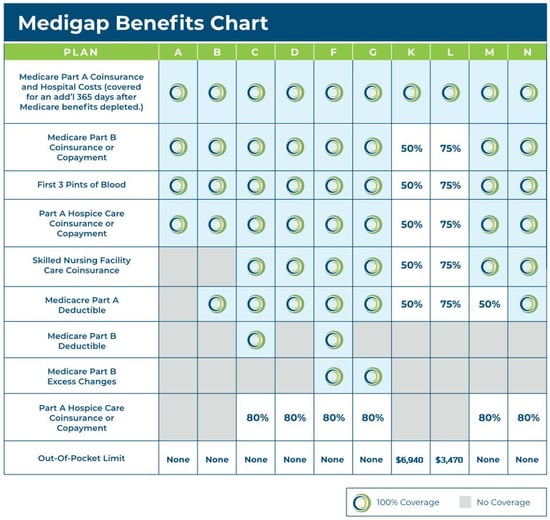
Plan F and Plan G are the two most popular Medigap plans, although Plan F (and Plan C) is no longer available to new Medicare enrollees who have become Medicare eligible after January 2020. As you can see in the Medigap comparison chart, Plan F covers all the gaps in Medicare. Plan G is only slightly different, so it is also a popular.
When you compare Plans F and G side by side, you’ll immediately notice that Plan G has only one difference which is the Part B deductible. If you compare annual premiums for Plan G and the premiums save you more than you will pay out for the Part B deductible, then enrolling in Plan G makes sense.
In recent years, Plan N has gained in popularity. Plan N offers lower premiums if you are willing to do some cost-sharing. Unlike Plan F or G though, Plan N does not cover excess charges. You’ll want to read up on this and understand what that means. Medigap Plan F is also offered as a high-deductible plan by some insurance companies in some states. If you choose the high-deductible option, it means you must pay for Medicare-covered costs (coinsurance, copayments, deductibles) up to the deductible amount of $2,700 in 2023 before your policy will pay anything.
For Medigap Plans K and L, after you meet your annual out-of-pocket limit and your annual Part B deductible ($226 in 2023), the Medigap plan pays 100% of covered services for the rest of that calendar year.
Plan N pays 100% of the Part B coinsurance, except for a copayment of up to $20 for some office visits and up to a $50 copayment for emergency room visits that don’t result in an inpatient admission.
Medigap Plan G also has a high-deductible option. In 2023, the HDG deductible is $2,700.
In Massachusetts, Minnesota, and Wisconsin Medigap policies are standardized in a different way. Click here for information on Wisconsin, Minnesota, Massachusetts Medigap Comparisons
Once you determine which Medigap plan feels right for you, then you can shop rates. The Medicare Solutions Group makes this simple with a zip code specific customized rate comparison report that looks at the top 3-5 lowest priced carriers. We'll determine if you are eligible for a household discount too. Keep in mind we'll analyze the rate increase history as well as carrier financial ratings to make sure your choice is the right one.
Additional Medicare Supplement Plan Information
You can use your Medicare Supplement plan at any provider in the nation that accepts Medicare. This makes Medicare supplements great for travel or for people who live in more than one state throughout the year. Around 93% of all U.S. primary care physicians accept Medicare.
Medicare Supplements plans do not include retail drug coverage, so you’ll want to purchase a standalone Part D drug plan for your medications.
Keep in mind that when you compare Medicare Supplement insurance that these plans are standardized- each insurance company sets their own rates, but the benefits are the same across the board. A Plan G is a Plan G from any carrier.
You pay the private insurance company a monthly premium for your Medicare Supplement insurance policy in addition to the Part B premium that you pay to Medicare. The Part B premium for 2023 will be $164.90/month for most individuals but you can find your rate based on your income level here (Part B costs).
You can purchase a Medicare Supplement policy from any insurance company that is licensed in your state to sell one.
Factors to consider:
- Eligibility for household discount
- Insurance company rate increase history
- Insurance company financial ratings
Calculate Cost Estimates
The amount that you will pay for Medicare each month will vary based upon your income and the kind of supplemental coverage you choose.
An example would be the base Part B premium of $164.90/month plus a Medigap Plan G monthly premium of $150/month plus a Part D premium of $32/month – your total would be $346.90/month in premiums.
With this example you can be sure your additional out-of-pocket spending would be minimal as Plan G would pick up the majority of your out-of-pocket costs.
There are many different Medicare plan options to choose from so that you can have a monthly premium within your budget.
Request a quote from The Medicare Solutions Group today!
Medicare Supplement Open Enrollment is a one-time window when you can enroll in any Medicare Supplement policy. You will not have to answer any medical questions. The Medicare Supplement insurance companies can’t turn you down during your Medicare Supplement Open Enrollment Period.
Keep in mind this period lasts for only 6 months, so be sure not to overlook this time unless you have other creditable coverage. Missing this Medigap Open Enrollment Period (OEP) can have future consequences such as higher premiums and limited coverage options.
It is important to note that your Medicare Supplement Open Enrollment Period is not the same as the open enrollment period that occurs each fall; as this can be confusing. Open Enrollment dates for Medicare Supplements vary for each person.

Open Enrollment Facts
- Only occurs once for most people
- Lasts for six months and then it is gone
- Once it’s gone, your opportunity for guaranteed issue is gone and then you must answer health questions to change plans in most states.
- People on Medicare under age 65 will get a rare second Open Enrollment for a Medicare Supplement later when they turn 65.
So if you don’t take advantage of your Medigap Open Enrollment window, you could find later on that you can’t medically qualify for a policy.
Open Enrollment Window Defined
Your personal Medicare Supplement Open Enrollment Period begins on the first day that your Part B becomes effective. If your Medicare Part A and Part B coverage starts on March 1st, then your personal enrollment period lasts for exactly 6 months and ends on August 31st.
Advantages to buying during Open Enrollment
The Medicare Supplement Open Enrollment Period is the only period you will ever have during which you can enroll in any Medicare Supplement plan. If you enroll during this period, you can choose any Medicare Supplement Plan– A, B, C, D, F, G, K, L, M or N.
Applications for Medicare Supplements generally have many medical questions. But, when you enroll within your 6 month window, you can avoid all the health questions on the application. The insurance company must accept your application and issue you the coverage when you apply during your Medicare Supplement Open Enrollment.
Once your Medicare Supplement Open Enrollment window ends, then the insurance company can require answers to health questions on an application. They can accept or deny your coverage based on your health. Some people may have health conditions which will prevent them from getting coverage later. This is why the Medicare Supplement Open Enrollment period is important for most people.
Medicare Advantage vs Medigap – how do you choose?
As you may know by now, Medicare alone doesn’t cover everything. Most people buy additional insurance to bridge the gaps. When considering Medicare Advantage vs Medigap plans, it’s important to understand that both types of plans will help to reduce your out-of-pocket spending.
After all, who wants to come up with a deductible each time you enter the hospital? Or pay 20% of the cost of an expensive MRI?
The two main types coverage that you can buy to help with this are Medicare Advantage vs Medigap (Medicare Supplement). It’s important that you know how each type of coverage works, so that you can select the right plan.
Medicare Supplements pay as a secondary insurance to Medicare itself. This means they pay after Medicare first pays its portion of the bill. You stay enrolled in Original Medicare, and Medicare sends the remainder of your bills to your Medicare supplement company. Then the supplement company pays its share according to which plan you are enrolled in.
You can see any provider that participates in Medicare, regardless of which supplement company you choose. You have access to all the Medicare providers nationwide – no referrals necessary. If you enroll in a comprehensive plan like Plan F or Plan G, you will have very little out of pocket cost.
When you enroll, your Medicare supplement insurance company notifies Medicare that you have purchased a policy. Then, when Medicare pays its portion of your bills, it will automatically send the remainder of your bill to your Medicare supplement company.
It’s seamless, with no claim forms for you to file.
Medicare Advantage Plans on the other hand, are entirely separate from Medicare. When you enroll into a Medicare Advantage policy, you get your benefits from the plan, not Medicare. You agree to use the plan’s network of providers except in emergencies. You’ll pay copays for your health care treatment as you go along.
These plans are an alternative to Original Medicare.
About 33% of beneficiaries choose to enroll into Medicare Advantage policies, which are private insurance plans. They usually have lower premiums than Medigap plan sometimes even a $0 premium on some plans in some areas.
When a plan has a $0 premium, it means that you will pay no additional premiums for the plan itself. You will still pay for your Part B premiums monthly. You must be enrolled in both Medicare Parts A and B to be eligible for a Medicare Advantage plan.
Why would any company offer a $0 premium plan? Because you agree to use the plan’s network providers to get your care. This means you’ll have substantially fewer doctors to choose from than if you chose a Medigap plan. The insurance company has more control over your choice of providers, with whom they negotiate contracted rates. Before choosing an Advantage Plan, check to see that your doctors are in the network.
Changing Between Medicare Advantage vs Medicare Supplement Plans
Many people wonder if they can start with Medicare Advantage and change to Medigap later if they get sick or need more coverage. It does not work that way. If you leave a Medigap plan to get Medicare Advantage coverage instead, you may not be able to get back into a Medigap plan later.
Can I change from Medicare Advantage to Medigap?
You might be outside of your one-time initial enrollment window by then, and that means Medigap plan insurance companies can ask health questions on your application. The insurance carriers can decline you for certain health conditions or even medications that you take, so be aware of this before changing to Medicare Advantage.
An exception: There is a trial period for people who try Medicare Advantage for the first time. If you decide to dis-enroll from the plan and go back to Original Medicare within the first 12 months of Medicare Advantage coverage, then you can return to your Medigap plan with no underwriting. After the 12 months is up, then you are subject to underwriting.
Some of the key factors for comparison are:
- Monthly premiums
- Deductibles, if any
- Expected costs of healthcare services on each plan
- How often you use healthcare services
- Areas where you will need access to care
- Expected copays for your medications
- Potential out of pocket spending for you on each plan type
Seem overwhelming? Have The Medicare Solutions Group team help you in your search with doctor networks and drug formularies to come up with the ideal plan for you.
Get In Touch With Us
No matter what, we're here to help. Send us a message and an experienced agent will be in touch with you to help answer your questions.



